During in vitro fertilisation, eggs are removed from the ovaries and fertilised with sperm outside the woman’s body, in a laboratory. One or more fertilized eggs (embryos) are then placed in the uterus.
The process
Exactly how the IVF process is carried out can vary somewhat between different clinics, and individual considerations can also serve to alter the procedure. Below, you will find one example of how an in vitro fertilization can be done.
1) Suppressing the natural menstrual cycle
The woman is administered a medicine that will suppress her natural menstrual cycle. The medicine is typically given as a daily nasal spray or as daily injections, and the treatment will continue for approximately two weeks.
2) Follicle stimulation
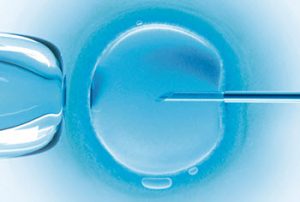 When the woman’s natural cycling has been suppressed, she will be given a follicle stimulating hormone (FSH) that encourages the ovaries to get more eggs ready than normally. It is administered in the form of injections, typically once a day for 10-12 days.
When the woman’s natural cycling has been suppressed, she will be given a follicle stimulating hormone (FSH) that encourages the ovaries to get more eggs ready than normally. It is administered in the form of injections, typically once a day for 10-12 days.
The FSH is intended to increase the number of eggs that will be ready for collection.
Throughout this treatment, vaginal ultrasound scans are performed to check on the condition of the ovaries. Blood tests can also be necessary. When it is 34-38 hours left before the eggs are to be collected, the woman receives a final hormone injection to help the eggs mature.
3) The sperm
If fresh sperm is to be used, the man will deposit sperm at the IVF clinic around the time when the eggs are being collected. The sperm will be washed and spun at a high speed to select the healthiest and most active sperm.
If frozen sperm is to be used, the clinic will thaw the sperm at the ideal time prior to fertilization. The thawed sperm will be washed and spun at high speed just like fresh sperm.
4) Egg collection
A needle is passed through the vagina and into each ovary, where the eggs are collected. The whole procedure typically takes 15-20 minutes and is normally done while the woman is sedated. Examples of side effects are cramps and vaginal bleeding after the procedure. Also, the sedation itself is always linked to certain risks.
5) Fertilization
The collected eggs are mixed with the sperm in the laboratory. After 16-20 hours, it is possible to see of the eggs have been fertilized.
N.B! In some cases, simply mixing eggs with sperm is not the best course of action. Instead, each egg is injected with a single sperm. This is called intra-cytoplasmic sperm injection (ICSI).
6) Embryo growth
Fertilized eggs (embryos) will be allowed to grow in the laboratory for up to six days.
7) Preparing the uterus
The woman will be given hormone medicines to encourage the uterus to get ready for receiving an embryo. The medicine can be an injection, a gel or a pessary (a pessary is inserted into the vagina).
8) Embryo selection
The best embryos will be selected for implanting. Nowadays, it is very common to select just one or two embryos even if there are several viable embryos available.
The rules or guidelines for how many embryos that will be selected and implanted varies depending on where you do your IVF. There can be national laws to adhere to as well as policies adopted by the individual clinic.
In many clinics, women under 37 years of age who go through their first IVF cycle will only have one embryo transferred. For women 37 years or older, or women who have already gone through their first IVF cycle, transferring two embryos is more common, especially if none of the available embryos are of the highest quality.
Viable embryos that aren’t selected for transfer can be frozen and saved for future IVF attempts.
9) Embryo transfer
The embryo is transferred to the uterus inside a catheter that is passed through the vagina. There is usually no need to sedate the woman for this procedure.
 After the IVF
After the IVF
Roughly two weeks after the embryo transfer, the woman will have a pregnancy test. Some clinics want the woman to come in for a blood test, while others recommend a standard urine test that can be done at home.
If the pregnancy test is positive, one or more ultrasound scans will be carried out during the following weeks to check if the pregnancy is progressing as expected. After IVF treatment, there is an increased risk for ectopic pregnancy, a condition where the embryo implants in the fallopian tubes instead of in the uterus. Examples of symptoms are stomach pain, dark vaginal discharge and vaginal bleeding.
Chances of an IVF treatment resulting in live birth
The chance of success can be impacted by various factors, including the cause of the infertility (male, female or both), the age of the woman and underlying health issues. Generally speaking, younger women are more likely to have a successful pregnancy after IVF than older women.
Percentage of IVF treatments that resulted in live birth:
32.2% for women under 35 years of age
27.7% for women aged 35-37
20.8% for women aged 38-39
13.6% for women aged 40-42
5% for women aged 43-44
1.9% for women aged over 44
Statistics for the year 2010, published by NHS UK.
Side effects of IVF treatment
IVF treatment can come with a number of side effects for the woman. This includes side effects from the medication, side effects from the egg collecting procedure and side effects from the transferring of the eggs into the uterus. IVF also increases the risk of ectopic pregnancy.
If more than one embryo is transferred into the uterus, there is a chance of multiple births such as twins or triplets. Twin pregnancy, triplet pregnancy and so on are associated with increased health risks for the mother and the children regardless of if it occurs naturally or is the result of IVF. Problems more commonly associated with multiple births include miscarriage, gestational diabetes, anaemia, heavy bleeding, pregnancy-related high blood pressure, and pre-eclampsia. The risk of needing a caesarian section is also greater. The children are more likely to be born prematurely and/or with a low birthweight, and the risk is also increased for conditions such as NRDS and cerebral palsy.
Medication side effects
Examples of common side effects to the medications used during IVF treatment are headaches, fatigue, hot flushes, feeling sad, feeling irritated, and feeling restless. There is also an increased risk of ovarian hyperstimulation syndrom.
Ovarian hyperstimulation syndrome (OHSS) is a condition where the medicine given to increase egg production works to well and too many eggs develop in the ovaries, causing the ovaries to become abnormally large. The symptoms can include ovarian pain, bloating, shortness of breath, and feeling faint. When OHSS occurs, it usually occurs in the week after egg collection. It is a serious condition. A woman experiencing symptoms of OHSS before or after egg collection should contact her IVF clinic immediately.
